What is osteoarthritis (OA)?
Osteoarthritis, the most common form of arthritis, often affects the hip joint.
Normally, smooth cartilage covers the ends of bones, allowing frictionless movement and absorbing stress. The hip also contains labral cartilage, which helps distribute weight and adds joint stability. In OA, this cartilage becomes thinner and rougher, causing pain, stiffness, and reduced mobility. While it can affect anyone, it’s more common in women over 50.
OA can be diagnosed by a qualified healthcare professional, based on your symptoms, without needing X-Rays or scans.
Contributing factors
- Previous injuries – Injuries or other joint conditions, such as gout, slipped capital femoral ephysis (SCFE), developmental dysplasia of the hips (DDH), perthes and femoroacetabular impingement (FAI) can increase your risk.
- Weight – Being overweight can significantly increase the stress on your hip joint.
- Age – Your risk increases as you get older, especially over the age of 45.
- Family history – OA may run in families, although studies have not identified a single gene responsible.
How will it affect me?
If you have hip OA, you may experience pain and stiffness in one or both hips. This can be worse at the end of the day or with movement and often improves with rest. Morning stiffness is common, usually lasting less than 30 minutes.
Pain is often felt in the groin, outer hip, or buttock, and can spread to the lower back, thigh, knee, or even the shin. You may find it harder to dress, especially putting on shoes and socks, or get in and out of a car.
The hip may feel stiff, less mobile, or make creaking or crunching sounds. Pain can sometimes disturb your sleep, and symptoms often vary from day to day.
Reduced use of the hip can weaken the surrounding muscles, making the leg look thinner and the joint feel unstable. Keeping these muscles strong is important to support your hip and prevent it from giving way.
Managing hip osteoarthritis
With some simple management approaches, you can reduce pain, stay active, and rely less on pain medication. Here's how:
Keep moving
Regular exercise keeps your joints healthy and muscles strong. The right balance of rest and activity is key - too much can worsen pain, too little can cause stiffness.
Strengthen muscles around your hip for better support. Aerobic exercise (like walking, swimming, or cycling) boosts fitness, eases pain, and improves sleep. Water-based exercise reduces joint strain while keeping you active. Aim for 2.5 hours of moderate aerobic activity each week, spread out over several days.
Manage your weight
Extra weight puts more strain on your hips, making it more likely that your OA will worsen. Follow a balanced, reduced-calorie diet with regular exercise to help manage your weight and ease symptoms. Your doctor can support you with weight loss advice.
Reduce strain on your hip
Pace yourself – spread out physical tasks and rest before pain worsens. Use a walking stick if needed, to take pressure off your hip.
Try heat or cold packs for pain relief (wrap them in a cloth and use for no more than 20 minutes). Wear supportive shoes to improve comfort and balance.
Look after your mental health and sleep
Pain and stiffness can affect your mood and sleep. Talk to your doctor if you're feeling low or anxious. Therapies like CBT or relaxation techniques may help.
For better sleep, keep a regular sleep schedule, limit screens before bed, or try a sleep diary to spot patterns. Your doctor or occupational therapist can offer more tips for better sleep.
Use pain relief wisely
Pain medication can help you stay active but won’t stop or cure the condition. Paracetamol or stronger painkillers (if prescribed) can ease discomfort. NSAIDs like ibuprofen reduce pain and swelling. Capsaicin cream (from chilli peppers) may help with local pain. Steroid injections may also provide short-term relief. Make sure you’re using pain relief safely under the guidance of your doctor.
What treatments should you not be offered?
According to the NICE guidelines (2022) the following treatments are not recommended for OA, as there’s little evidence they help:
injection of a substance called a hyaluronon into the affected joint
creams containing a substance called rubefacients
glucosamine or chondroitin products
acupuncture
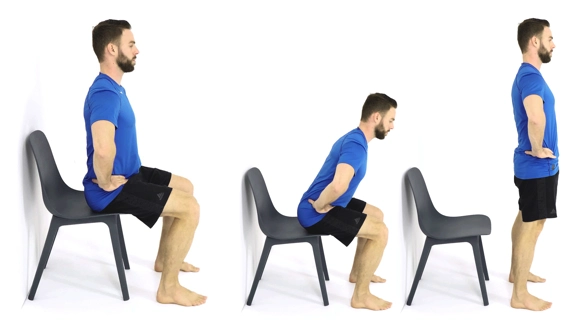
Exercises
These exercises are designed to keep your hip flexible and strong. Start small and build up over time, aiming to be consistent even if your symptoms reduce. It is normal to experience discomfort during or after exercise; reduce intensity if this becomes unmanageable.
How will physiotherapy help?
Physiotherapy can help identify and support your understanding of key contributing factors. Our aim is to work together to form a personalised rehabilitation programme guided by your symptoms, physical function and goals. We will focus on a combination of behaviour modification, knee strengthening exercises, weight management and pain management approaches.
It may take 3-6 months to notice changes, so it’s important to:
- remain consistent with your exercise and lifestyle routine, even if you notice an initial slight increase in symptoms
- keep going, even if you feel better, to reduce risk of symptoms returning or worsening
Physiotherapy has a range of options to support you, including:
- one-to-one appointments with a physiotherapist/assistant
- weekly group education and exercise classes
- patient-initiated follow-up review processes
- supported referral to local health and wellbeing schemes
Further information and support
Visit the Musculoskeletal Physiotherapy Outpatients service page on our website for information, resources, and self-referral support.
NHS Berkshire Talking Therapies
A free and confidential service offering effective treatment for common mental health problems such as low mood, stress, or worry. You can refer yourself or ask your GP or health professional to refer you.
Arthritis UK (formerly Versus Arthritis)
Free information on OA, including managing symptoms and flare-ups, specific types of exercise, benefits and limitations of OA management options, online support groups.
Nuffield Joint Pain Programme
Free 6-month rehabilitation programme for those living with OA. Includes bi-weekly education and exercise sessions, plus supported gym work and advice. Self-refer on their website.
Related services
Musculoskeletal Physiotherapy Outpatients
- Adults
Treatment plans to manage or improve musculoskeletal conditions, including chronic pain, recovery from surgery, and osteoarthritis.
Musculoskeletal Physiotherapy Outpatients: Go to serviceCommunity Physiotherapy Service (East Berkshire)
- Adults
Support at home for housebound adults who are unable to attend clinic appointments, including a personalised rehabilitation plan.
Community Physiotherapy Service (East Berkshire): Go to serviceTalking Therapies
- Adults
A free and confidential service offering effective treatment for common mental health problems such as low mood, stress or worry.
Talking Therapies: Go to service