Overview
Plantar heel pain (often referred to as plantar fasciitis) is when you have pain on the bottom of your foot around your heel and the arch of your foot.
Signs and symptoms
This condition generally starts with pain under the heel or ball of your foot. It is the irritation of the fibrous band under the foot, called the plantar fascia, that connects your toes and heel bone.
It’s often made worse by long periods of standing and walking and may also be acutely painful on first stepping on the heel after periods of rest, such as stepping out of bed in the morning.
This heel pain can be caused by:
- being overweight
- prolonged periods of standing
- sudden increases in activity
- prolonged activity with minimal rest periods, such as long-distance running
Contributing factors
Several factors can make the plantar fascia more sensitive, including:
- being aged 40-60
- being female
- diabetes
- inflammatory conditions, such as rheumatoid arthritis or ankylosing spondylitis
- foot type – high‑arched feet may increase stress on the plantar fascia
- tight calf muscles or reduced ankle movement
- worn‑out or unsupportive shoes
Treating heel pain
Treating the pain may take some time. These suggestions may help.
If your symptoms continue, please speak to your GP, who may refer you to a physiotherapist or podiatrist.
- Modify your activities – Reduce or avoid running, excessive walking, and standing for longer periods
- Apply ice – Use a cold bottle or can from the freezer and roll it along the bottom of your foot for up to 10 minutes. Wear a thin sock to protect your skin, and do not do this if your sensation is impaired
- Footwear – Wear supportive shoes with a firm sole, cushioning, and good arch support (running trainers work well). Avoid going barefoot or wearing flip‑flops
- Medications – Pain relief can be helpful, but speak to your GP or pharmacist for advice
- Weight management - Extra weight increases strain on the plantar fascia. Losing even a small amount can reduce symptoms
- Insoles (orthoses) – Arch‑supporting insoles may reduce pain. Try ‘off‑the‑shelf’ options first. If needed, you may be referred to a podiatrist or orthotist for custom insoles
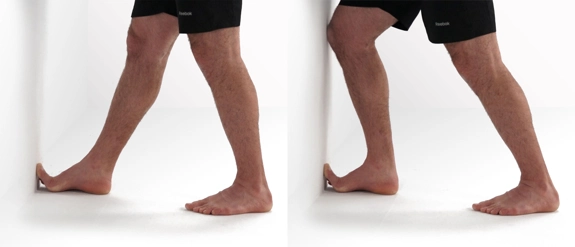
Exercises
Complete these gentle exercises little and often to help reduce stiffness and other symptoms. They may be uncomfortable, but they should not significantly increase your symptoms.
When to seek help
If you feel these exercises are making your symptoms worse, take a break. You can also speak to your GP for further help. This doesn’t mean it’s anything too serious. It may be that you need some extra help to deal with the symptoms, and you may be referred to a physiotherapist.
Related services
Musculoskeletal Physiotherapy Outpatients
- Adults
Treatment plans to manage or improve musculoskeletal conditions, including chronic pain, recovery from surgery, and osteoarthritis.
Musculoskeletal Physiotherapy Outpatients: Go to serviceCommunity Physiotherapy Service (East Berkshire)
- Adults
Support at home for housebound adults who are unable to attend clinic appointments, including a personalised rehabilitation plan.
Community Physiotherapy Service (East Berkshire): Go to servicePhysiotherapy Service for children and young people
- Children & young people
Help for children and young people up to the age of 19 who have difficulties with gross motor skills, including posture and mobility.
Physiotherapy Service for children and young people: Go to service